Opinion: Editor Claire on living with her brain injury
This March is Brain Injury Awareness Month, to help raise awareness about the impact brain injuries have on individuals and their families. Want to know what life’s like after a brain injury, especially when people think you’re fine five years on? Here’s my story – and how things will never be the same. And I’m one of the lucky ones.
This article contains sensitive content surrounding illness and mortality, as well as an image which some readers may find triggering or distressing.
Meningitis. Heard of it, right? Encephalitis? Nope? Neither’s 77% of the world, says Encephalitis International. Neither had I. Until I woke up in hospital after 15 days on life support.
What is encephalitis? While meningitis is an inflammation of the protective membranes surrounding the brain, encephalitis is an inflammation of the brain itself. It’s caused either by an infection, or through the immune system attacking it in error. In the UK each year there are up to 6,000 cases, with a mortality rate up to 40%. Death is usually caused by severe brain swelling, resulting in pressure on the brainstem. That’s the part that controls breathing and circulation – with it then ceasing to function. Cheery stuff, no? But it’s the stuff you need to know about. And I’m determined each year – as I have in magazines and on TV – to share my experience to help people know the early signs and how things can progress so quickly.
What are the symptoms? It depends on the type. It’s usually a flu-like illness or headache and high temperature. Then there’s uncharacteristic behaviour, seizures, and loss of consciousness. But symptoms alone are not enough of a diagnosis. Hospitals perform a variety of tests, such as brain scans, a spinal tap and EEG monitoring. Now, let’s talk about me, shall we?

I was all fine and dandy one minute back in June 2021 – then not so great the next. I caught a cold and kept complaining how tired I was. I’d sleep for hours. My husband, Scott – thinking I was in the midst of a nasty cold – packed me off to bed one night when I couldn’t even keep my eyes open to eat a bowl of soup. I fell asleep, and didn’t wake up.
Panic set in the next morning when Scott couldn’t rouse me. An ambulance was called, with my dad scooping my boys off to my parents. By this time I was semi awake, with our security cameras catching me stumbling into the back of the ambulance. When we arrived at our local hospital I sat in the A&E waiting room next to Scott, who’d arrived separately due to Covid restrictions. I then started having seizures, rendering me unconscious to the point I was put on a ventilator. The doctors no longer knew what to do, so I was transferred to The Royal London Hospital for specialist help. It was there that my diagnosis was confirmed. With my parents and Scott being told I may never wake again.
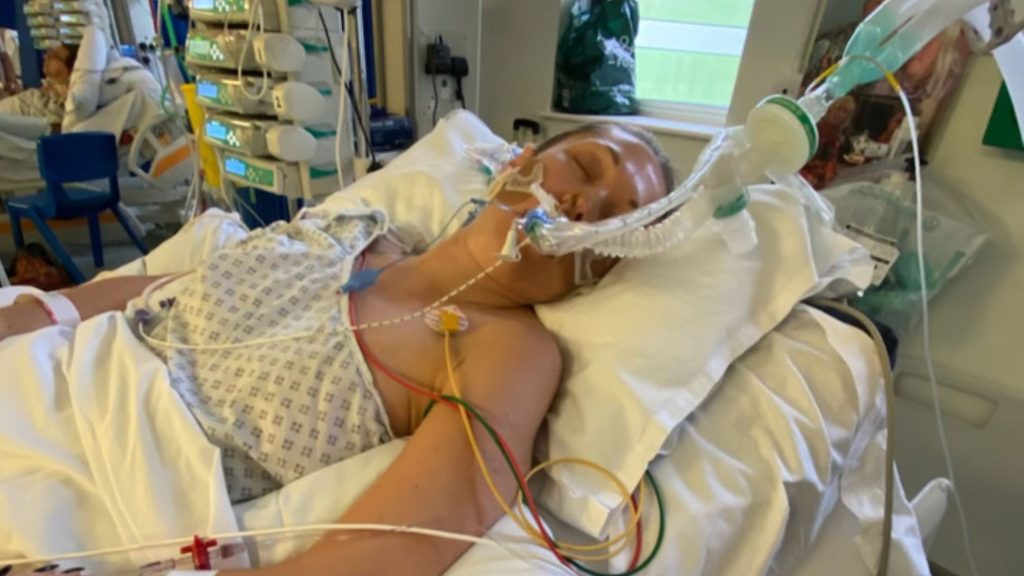
Obviously I did – how else would I tell this tale? – after 15 nights on life support. And while my family breathed a sigh of relief that I was conscious, it was clear things weren’t right. “How are the cats?” I asked. They’d passed away a few years earlier. “When can I speak to Auntie Karen and Uncle Peter?” My uncle died of a heart attack 10 years before. Encephalitis had damaged the part of my brain that ‘stored’ memories. There was little hope of it returning (very much the case). I have no recollection of getting married, giving birth to my sons, 9/11 – everything from the last 25 years.
My family were also alarmed with the way I acted. “There’s flies in my ears and wasps in the ceiling,” I said to Scott one night. Another time he listened as I told him my father-in-law was sitting next to me laughing. He was at home 40 miles away. My mum brought in a picture of my boys, and the doctors kept asking what their names were and where they lived. I refused, because I was adamant they were going to be kidnapped at any moment. One thing I do recall is a nurse trying to give me my medication. Refusing, I spat in her face: I’ll never forget the look in her eyes. I was experiencing a type of Intensive Care Delirium – confusion, hallucinations, paranoia, and agitation, which eventually resided. And, after a further three weeks in hospital, I was well enough to be discharged.

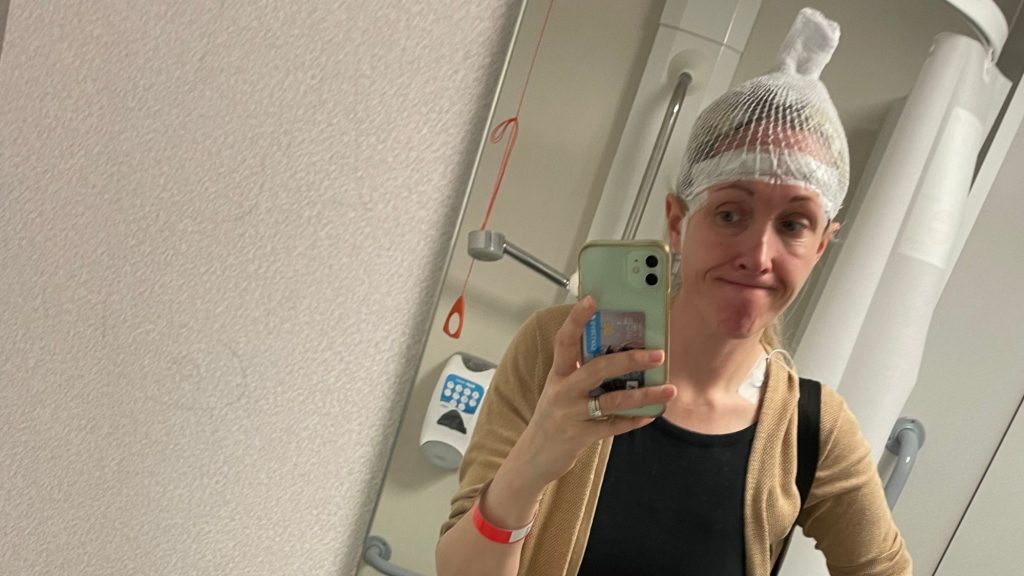
That’s the end of my story, surely? Nope. I’m now short-tempered. I’m now epileptic due to the seizures so can’t drive. I scream when my phone rings. No one can go near my right ankle as for no reason whatsoever it’s agonising to touch. I’ll often look in the mirror and see a woman with a bright red nose staring back – another attractive side effect, which my boys now refer to ‘Mum having a Rudolph moment’. Last year I had to stay at The Royal London for a week of brain monitoring. Not stylish, as you see below. I’m back this month for another week to see whether different meds could manage my seizures entirely. That means I could get my driving licence back. The question is, will I need lessons? I reckon so, especially when I recently told my husband at a roundabout to give way to the left. Oops.
I’m aware I’m making this sound light-hearted, but of course a brain injury isn’t. I’m one of the lucky ones. But it would be lovely to hop in the car to see friends. To not to have to write notes so I don’t forget what I’m doing. I’d like to open a web browser and not forget why I’ve opened it. And for Scott to not have to repeat the same answer I’d asked him about yesterday. Or the day before – and the day before that. I might look the same on the outside, but what people need to be aware of is that those who’ve suffered a brain injury are very much not the same on the inside. Because even though I’m trying to make it sound like a laughing matter, living with a brain injury is no laughing matter.
The information I am sharing is regarding my own experience with a brain injury. Specific, professional, or medical advice should always be sought from qualified specialists.
If you know someone who has recently sustained a brain injury, who is living with the long-term effects, or is experiencing grief following a brain injury click here to see the support available. For further emotional support call Samaritans free, day or night, on 116 123.






